Obstetrics
Posted On April 28, 2018 by Dr.Shobhana Mohandas
Click Here To Download
Natural menopause is associated with lack of functioning of ovaries, which are two hormone producing organs situated near the womb or the uterus. Normally, these ovaries produce 3 hormones,viz: oestrogen, progesterone and androgens. When they stop functioning, a woman faces many physical and mental changes
Polycystic Ovarain Syndrome
Posted On April 26, 2018 by Dr.Shobhana Mohandas
PCOD or polycystic ovarian syndrome is an enigmatic entity so far. The syndrome was first described in 1935 when American gynecologists Irving F. Stein, Sr., and Michael L. Leventhal associated the presence of ovarian cysts with anovulation. For many years these factors were used as the diagnostic criteria of the syndrome. A lot of research has been in place over last 78 years but till today the exact cause of the syndrome is not clear. Broadly there is a finding of multiple cystic changes in the periphery of the ovary. This is combined with hyperandrogenism and neuroendocrine manifestations of increased LH levels. It is considered to be a lifestyle disease. It is closely related to the metabolic syndrome associated with insulin resistance at tissue levels, with subsequent hyperinsulinemia. It affects a sizeable percentage of females.
Diagnosis
In 2003 a consensus workshop sponsored by ESHRE/ASRM in Rotterdam indicated PCOS to be present if any 2 out of 3 criteria are met.
- Oligoovulation and/or anovulation
- Excess androgen activity
- Polycystic ovaries (by gynecologic ultrasound)
- Other entities are excluded that would cause these
In 2006 the Androgen Excess PCOS Society suggested a tightening of the diagnostic criteria to all of:
- Excess androgen activity
- Oligoovulation/anovulation and/or polycystic ovaries
- Other entities are excluded that would cause excess androgen activity
Ultrasound crieteria: The Rotterdam consensus defined the polycystic ovary as having 12 or more follicles, measuring between 2 and 9 mm , and/or an ovarian volume >10 cm. Excess androgen activity: Excess androgen activity may be manifested as hirsuitism, acne, or androgen-dependent alopecia. Elevated levels of testosterone(abnormal ovarian androgen production) or Dehydroepiandrosterone(Increased adrenal production of androgen) are biochemical markers of hyperandrogenism. Etiopathology of PCOS: PCOS is a familial condition. It can have a genetic etiology, with an autosomal dominant mode of inheritance. Girls with low birth weight as well as a family history of diabetes mellitus or premature cardiovascular disease are at high risk for developing PCOS.
Many pathophysiologic hypotheses have been proposed to explain the clinical findings of PCOS.
- The neuroendocrine defect
- The insulin hypothesis
- The ovarian hypothesis, a primary defect of sex steroid synthesis or metabolism results in exaggerated ovarian androgen secretion and anovulation.
- A fourth hypothesis for a primary defect at the level of the ovary comes from the classic polycystic ovary morphology seen
- Inflammatory markers are increased in PCOS1.
Neuro endocrine hypothesis2 Gradual increase in testosterone levels during pubertal progression may gradually impair progesterone inhibition of daytime GnRH in girls who develop PCOS .This leads to increased GnRh/LH pulses. In ovulatory cycles there is a slowing of GnRh pulse during the luteal phase in response to increased progesterone levels.. In contrast to this, in PCOS patients there is a persistently rapid GnRh pulse frequency even in the luteal phase. This is because of impaired sensitivity of the GnRH pulse generator to suppression by progesterone. The persistently rapid GnRH pulse frequency favours LH production over FSH. Under normal circumstances, the theca cells of the ovarian follicles produce androgens under the control of LH. These androgens are then aromatized into estrogens, primarily estradiol, by the adjacent granulosa cells. FSH stimulates the granulosa cell growth and aromatase capacity. In PCOS there is increased LH pulsefrequency. This induces theca cells to produce more androgens. The relative FSH deficiency also interferes with granulosa cell aromatization to estrogens in the ovary and impairs follicle maturation and ovulation. The increased production of androgens by the theca cells further makes the GnRh pulse regulator more insensitive to progesterone and the cycle of anovulation continues further.
The Insulin Hypothesis: In women with PCOS, basal insulin secretion is increased and hepatic insulin clearance is reduced, resulting in hyperinsulinemia. There is also impaired suppression of hepatic gluconeogenesis. Inhibition of hepatic production of sex hormone binding globulin further increases circulating free testosterone levels. The insulin receptor belongs to a family of tyrosine kinase receptors, including insulinlike growth factor- 1 (IGF- 1) receptor. Elevated serum concentration of insulin could act directly via the IGF-I receptor to increase androgen production. Ovarian theca cells are directly induced to produce more testosterone. It is interesting that in contrast to adipocytes and muscles, ovarian cells are insulin sensitive and allows insulin to activate it’s homologous receptor, resulting in androgen production. PCOS patients show decreased glucose transport in adipocytes. Further, insulin resistance in PCOS adipocytes leads to increased circulating Free Fatty Acid levels that, in turn, produce peripheral insulin resistance. There is impaired glucose transport into the muscles, reduced by 35-40%, due to reduction in Insulin-stimulated activation of PI3-kinase. This is independent of obesity. As a result, the glucose in blood remains elevated for a longer time and further stimulates pancreatic beta cells. These cells enhance their secretion of insulin to improve glucose uptake in muscles.
Low-grade inflammation in polycystic ovary syndrome: Recent evidence indicates a condition of low-grade chronic inflammation in PCOS that could be considered one of the potential links between PCOS and long-term metabolic (type 2 diabetes) and cardiovascular complications.3 Many studies have demonstrated that in women with PCOS a positive relationship exists between CRP values and insulin resistance, body weight and fatty mass. CRP is a classic marker for low grade inflammation. Other classic markers that are elevated are IL-18 and TNFα. Adipose tissue secretes several adipocytokines that, together with adipocyte
hypoxia and subsequent necrosis, draw many inflammatory cells, such as monocytes and T cells. A vicious circle is established with a continuous release of inflammatory mediators that are responsible for the development of insulin resistance, dyslipidemia, endothelial dysfunction, and metabolic and cardiovascular long-term complications. In addition, inflammation also has an impact on the regulation of the synthesis and secretion of androgens in the ovary and in the adrenal, contributing to the maintenance of the syndrome.
Clinical Evaluation of PCOS
Patients with PCOS may have oligomenorrhea (i.e., menstrual bleeding that occurs at intervals of 35 days to 6 months, with 9 menstrual periods per year) or secondary amenorrhea (an absence of menstruation for 6 months). PCOS may manifest itself as early as the first decade of life by premature pubarche or menarche. Oligoamenorrhea, although very common soon after menarche, may be an early symptom of PCOS, especially in overweight girls with hirsutism or acne. It has been suggested that in adolescents, all 3 elements of Rotterdam criteria should be fulfilled in this group for diagnosis of PCOS. In the reproductive age, Infertile patients may have hypothyroidism or hyperprolactinaemia or diminished ovarian reserve which can cause abnormalities in menstrual pattern and should be differentiated from PCOS.
- • Heavy menstrual bleeding may be present . Differentiation from other causes of abnormal menstruation has to be kept in mind while evaluating the patient
- • Hyperandrogenism clinically manifests as excess terminal body hair in a male distribution pattern. Hair is commonly seen on the upper lip, on the chin, around the nipples, and along the linea alba of the lower abdomen.
- • Some patients have acne and/or malepattern hair loss (androgenic alopecia). It should be differntiated from normal
- • In the extreme form of PCOS termed hyperthecosis, there may be, clitoromegaly, increased muscle mass, voice deepening,
Infertility: Infertility may be the presenting complaint in PCOS. Other causes of anovulation have to be ruled out in these patients. PCOS women also tend to have miscariage, and may require continuation of treatment with insulin sensitisers even after conception, to prevent miscarriage. Obesity and metabolic syndrome: Approximately 50% of women with polycystic ovarian syndrome (PCOS) have abdominal obesity,
characterized by a waist circumference greater than 35 inches (> 88 cm). It may also be part of metabolic syndrome which many patients with PCOS suffer from. Women with PCOS have an increased prevalence of coronary artery calcification and thickened carotid intima media, which may be responsible for subclinical atherosclerosis. Approximately 10% of women with PCOS have type 2 diabetes mellitus, and 30-40% of women with PCOS have impaired glucose tolerance by 40 years of age. Sleep apnea: Many women with PCOS have obstructive sleep apnea syndrome (OSAS), which is an independent risk factor
Investigations
- Exclude pregnancy as cause of amenorrhoea.
- Ultrasonography: Not mandatory if diagnosis is made clinically and biochemically. polycystic ovary is diagnosed as one having
- Serum Testosterone: Mean levels in PCOS are in the range of 60–80 ng/dL and are unlikely to exceed 150 ng/dL. Circulating bioavailable testosterone levels are usually elevated, while total testosterone may be normal due to low levels of sex hormonebinding globulin. Oral contraceptives, normalize the levels of circulating androgens in women with PCOS. Recommended Investigations after Diagnosis
- Blood glucose levels: to check for glucose intolerance.
- FSH and LH levels: An increased ratio of luteinizing hormone to follicle-stimulating hormone >2 is found in 60 to 70% of women
- Thyroid levels: Thyroid abnormalities to be excluded as cause for menstrual abnormalities.
- Oestradiol and FSH levels: High FSH means premature ovarian failure.
- 17- hydroxyl progesterone: To rule out late onset adrenal hyperplasia.
- DHEAS: A marker for adrenal androgen production. Elevated in adrenal tumours.
- • Androstenedione: Elevated in ovarian androgen secreting tumours 24 hour urine
abdominal obesity (waist circumference >35 in), dyslipidemia (triglyceride level >150 mg/dL, high-density lipoprotein cholesterol [HDL-C] level < 50 mg/dL), elevated blood pressure, a proinflammatory state characterized by an elevated C-reactive protein level, and a prothrombotic state characterized by elevated plasminogen activator inhibitor-1 (PAI-1) and fibrinogen levels. Insulin levels need not be tested to determine hyperinsulinemia.
Management of PCOS
Lifestyle modifications: In obese women with PCOS, even if medications are given, life style modifications by way of exercise and a diet plan is essential to minimise lipid irregularities and decreasing insulin resistance and the levels of testosterone, insulin, and luteinizing hormone in the body.
Insulin sensitizers: When administered to insulin-resistant patients, these drugs act to increase target tissue responsiveness to insulin and thereby reduce the stimulus for compensatory hyperinsulinemia. Metformin: Metformin is a second-generation biguanide. The drug activates glucose transporters to facilitate passage of glucose into hepatic and muscle cells, thereby decreasing peripheral insulin resistance and lowering serum glucose levels4. In general, clinical studies have shown that metformin treatment (500 mg three times per day or 850 mg twice daily with meals) increases the frequency of spontaneous ovulation, menstrual cyclicity, and ovulatory response to clomiphene citrate (CC) in women with PCOS. Metformin does not stimulate insulin release and, when administered alone, does not cause hypoglycemia. Side effects of metformin include gastrointestinal symptoms (e.g., nausea, vomiting, and diarrhoea) that are dose-dependent and generally tend to resolve after several weeks of treatment; a gradual increase in dose also helps to improve tolerance. Lactic acidosis is a rare but serious potential adverse effect of metformin therapy. Therefore, metformin should not be prescribed to patients with renal, hepatic, or major cardiovascular disease or hypoxia because such patients are predisposed to elevated lactate levels. Precautionary temporal withdrawal of metformin is advised for patients scheduled for surgery or for radiologic procedures involving the use of intravascular iodinated contrast.
Other Drugs used in the Management of PCOS Raloxifene
Raloxifene is a SERM approved for the treatment of osteoporosis in postmenopausal women , with antiestrogenic effects at the level of the hypothalamus and/or pituitary similar to CC. Raloxifene may have a favorable impact on markers of endometrial receptivity compared with CC, and it has been shown to increase FSH levels in premenopausal women. Ernesto de Paula Guedes Neto et al5 have, in a study, proved that 100 mg of Raloxifene for five days is as efficacious as clomiphene in inducing ovulation, with a more favourable effect on the endometrium.
Pioglitazone
Hyperinsulinemia caused by insulin resistance in PCOD causes hyperandrogenemia. Metformin is traditionally used to improve this resistance and lower the blood glucose levels. However, many patients cannot tolerate the side effects of Metformin and some are resistnant to it. Pioglitazone is another insulin sensitizing agent which can be used to improve ovulation in PCOS. Its action is different from Metformin. It acts after insulin binding by insulin receptors to improve the action of insulin, reduces its resistance to hormones, and inhibits glucose production in the liver3. pioglitazone may be effective in cases of dexamethasone- or metformin-resistant PCOS in the dose of 30 mg per day.
Atrovastatin and Simvastatin7,8
The cholesterol lowering Statins, Atorvastatin in the dose of 20 mg or Simvastatin 20 mg per day has been found to be effective in reducing inflammation, biochemical hyperandrogenemia, and metabolic parameters in patients with PCOS after a 12-week period. Homocysteine levels have also been found to be lower with the use of Statins in PCOS patients.
Insositol
The inositol phosphoglycans (IPGs) are putative mediators in a nonclassic insulin signaling cascade for glucose uptake and use. Insulinresistant women with PCOS display decreased insulin stimulated release of d-chiro-inositol (DCI)-containing IPGs (DCI-IPGs) during an oral glucose tolerance test (OGTT), which was related to impaired coupling between insulin action and the release of the DCIIPG. Oral nutritional supplementation with inositol, part of the vitamin B complex (B8) and an intracellular second messenger, was demonstrated to enhance insulin sensitivity and improve the clinical and hormonal characteristics of patients with PCOS.9 Treatment of PCOS patients with myoinositol in one study provided a decreasing of circulating insulin and serum total testosterone as well as an improvement in metabolic factors10. 2g myoinositol twice daily can improve oligomenorrhea, and ovulation in PCOS patients. Continued treatment may also result in significant weight loss (and leptin reduction) and an associated change in HDL cholesterol11.
Multivitamins
Jorge et al,12 in a prospective study concluded that consuming multivitamin supplements at least three times per week was associated with a reduced risk of ovulatory infertility. This association appeared to be mediated in part by folic acid. Vitamin D3 Selimoglu et al have, using a single dose of 300,000 units of 25-hydroxyvitamin vitamin D3 orally, in PCOS women in a study, concluded that PCOS women are mostly deficient in vitamin D3 and supplementing them with vitamin D3, can have a beneficial effect in improving insulin resistance in obese women with PCOS13 .
N-Acetyle Cysteine
N- acetyle cysteine as an adjunct to clomiphene citrate or Metformin could improve insulin sensitivity in PCOS subjects14,15,16. 1.8 gm/day in normal weight women (600 mg three times a day) and 3 gm/day in extremely obese women for 5 to 6 weeks are the dosages recommended.
PCOS in the Adolescent
If hyperandrogenism is the presenting complaint, OC pills containing cyproterone acetate for 6 months are found to be effective in decreasing signs of hyperandrogenemia Testing in adolescents presenting with PCOSlike symptoms is given in Table 1. In patients with associated obesity diet and exercise are mandatory. Metabolic syndrome is also becoming increasingly common adolescents.
The reduction of bodyweight in this young age group may require the collaboration of the pediatrician, dietitian, and sychotherapist. Adolescents with isolated cycle irregularity may be placed on a cyclical progestin regimen to induce withdrawal bleeding. Metformin, by decreasing insulin resistance, alleviates many of the hormonal disturbances and restores menses in a considerable proportion of patients. It may be used alone or in combination with oral contraceptives. In patients who cannot tolerate Metformin, alternative therapy like myo-inositol can be considered. Independently of medical treatment, restoration and maintenance of bodyweight within normal range is of paramount importance.
Conclusion PCOD is an enigmatic disease. Life-style modifications form an important aspect of treatment. Symptomatic treatment for presenting complaints like infertility, hirsuitism, and irregular menstruation will be necessary. Metformin is useful in lowering insulin levels, but all patients may not tolerate it. Adjuvant treatment with many agents have been found useful, but the number of studies with these agents are not very large.
Nutriction Suppliments In Obstetrics and gynacology
Posted On April 26, 2018 by Dr.Shobhana Mohandas
Various nutritional supplements are today being studied in the management of a variety of conditions, like infertility, recurrent abortions, and pre-eclampsia. Controlled studies are not available about the efficacy of many of these products. They are marketed by various pharmaceutical companies, promising dramatic improvement. The dose of many of these nutritional supplements is still not known/standardized, as studies to prove their efficacy are still going on. What follows is an overview of the various nutritional supplements used in the field of Obstetrics and Gynaecology.
Anti-oxidants
Antioxidants are broadly substances which reduce the oxidative damage caused by reactive oxygen species, which are free radicals. Free radicals are molecules or atoms that contain unpaired electrons. These are extremely unstable and will almost instantly capture electrons from nearby molecules, destabilizing them. Free radicals are formed naturally in the body during metabolism.
Reactive oxygen species (ROS) are highly reactive oxidizing agents belonging to the class of free radicals. Free radicals are molecules or atoms that contain unpaired electrons. These are extremely unstable and will almost instantly capture electrons from nearby molecules, destabilizing them. They are formed naturally in the body during metabolism.
Free radicals in the form of ROS can modify cell functions; endanger cell survival, or both. Hence, ROS must be inactivated continuously to maintain only the small amount necessary to maintain normal cell function. Free radicals could have the following implications in the field of obstetrics and gynaecology:
- The production of excessive amounts of ROS in semen can overwhelm the antioxidant defense mechanisms of spermatozoa and seminal plasma causing oxidative stress.
- Reactive oxygen species (ROS) have been implicated in diabetic embryopathy.
- Oxidative damage has been implicated in preterm premature rupture of membranes (PPROM).
- Increases in oxidative stress have been associated with intrauterine growth restriction (IUGR).
- A sharp peak in the expression of the markers of oxidative stress in the trophoblast was detected in normal pregnancies and this oxidative burst if excessive was speculated as a cause of early pregnancy loss.
Types of anti-oxidants: While vitamins A, C, and E have been recognized for a long time for their antioxidant properties, there are others such as zinc, selenium, and bioflavonoids which directly or indirectly serve as free radical scavengers.
Vitamins E & C Vitamin E, discovered in 1922, is the name given to a group of naturally occurring lipid-soluble antioxidants, the tocopherols and the tocotrienols, that are found in certain plant oils31. Vitamin E is the major, if not the only, chain-breaking antioxidant in membranes. The recommended dose of Vitamin E in human pregnancy is 22–30 mg/day.
In Preecclampsia: Two large, prospective, randomized trials involving more than 4000 low and high-risk subjects, respectively, compared vitamin C/E to placebo. There were no differences noted in the frequency of preeclampsia between groups 3. High doses of vitamin C(>500mg) and high doses of vitamin E(>400IU) have been known to be detrimental to pregnancy1.
USG taken 2 days later showed resolution of the fluid and the patient remained asymptomatic thereafter. Thus, even if fluid is seen in the pouch of douglas after injection of methotrexate, if it is not of a large amount, one need not worry.
In a randomized controlled study of 81 women who were at high risk for developing preeclampsia ( Women were identified as “at-risk” by a history of preeclampsia that required delivery before 37 weeks of gestation in the preceding pregnancy or by abnormal uterine artery Doppler FVW (resistance index of >=95th percentile for gestation or the presence of an early diastolic notch at 20 weeks of gestation)and who were taking vitamin C 1000mg and Vitamin E 400mg, Chapel LC et al concluded that administration of vitamin C and E from 16-22 weeks of pregnancy , was beneficial in preventing preeclampsia. However, in a similar study on1977 woman, In the Australian Collaborative Trial of Supplements (ACTS), did not find any difference between women who were treated with vitamins C & E and those who were not. The results of these 2 workers using vitamin E in the dose of 400mg and Vitamin C in the dose of 1000mg in preventing preeclampsia in high risk populations have conflicting results. However, the Indian gynaecologist would do well to note the dose of the vitamins used by these workers to achieve their ends. India also may boast of higher number of susceptible populations compared to our western counterparts. If any gynaecologist wants to try out these vitamins to prevent preeclampsia, they should probably be used in the same dose that these workers have used. It should also be remembered that vitamin E which was considered an innocuous drug so far should not be used in very high doses for long periods of time.
The results of these 2 workers using vitamin E in the dose of 400mg and Vitamin C in the dose of 1000mg in preventing preeclampsia in high risk populations have conflicting results. However, the Indian gynaecologist would do well to note the dose of the vitamins used by these workers to achieve their ends. India also may boast of higher number of susceptible populations compared to our western counterparts. If any gynaecologist wants to try out these vitamins to prevent preeclampsia, they should probably be used in the same dose that these workers have used. It should also be remembered that vitamin E which was considered an innocuous drug so far should not be used in very high doses for long periods of time.
In Male infertility: Rolf et al performed a placebo controlled, double-blind study of high dose oral vitamins C(1000mg) and E(800mg) for 56 days in 31 infertile men with asthenozoospermia and a normal or only moderately decreased sperm concentration25. They concluded that combined high-dose antioxidative treatment with vitamins C and E did not improve conventional semen parameters or the 24-h sperm survival rate. Since vitamin C and E in very high doses have been shown to have little or no effect on oligoasthenospermia, it probably is of no use in male infertility and certainly there may be no rationale in increasing the cost of a tablet by incorporating vitamin E or C in it in small doses with the hope of enhancing the role of the primary drug.
Female infertility: As oxidative stress results in luteolysis, antioxidant supplementation, for example vitamin C and vitamin E, has been shown to have beneficial effects in preventing luteal phase deficiency and resultant increased pregnancy rate and others have reported no value. Improved pregnancy rates were also reported with combination therapy with the antioxidants pentoxifylline and vitamin-E supplementation for 6 months in patients with thin endometria who were undergoing IVF with oocyte donation.
Zinc Dietary studies typically estimate usual zinc intakes of pregnant women throughout the world to range from 5 to 15 mg/day, compared with a 1989 US Recommended Dietary Allowance of 15 mg/day during pregnancy2. Severe maternal zinc deficiency is associated with infertility, spontaneous abortion, and congenital malformations, including neural tube defects. Maternal zinc deficiency has been associated with low-birth-weight (LBW), intrauterine growth retardation (IUGR), and preterm delivery.
Daily zinc supplementation in women with relatively low plasma zinc concentrations in early pregnancy is associated with greater infant birth weights and head circumferences, with the effect occurring predominantly in women with a body mass index less than 26 kg/m2.8 However, Mahomed in a systematic review of 7 trials found no difference on small for gestational age fetuses (SGA) between the group receiving zinc and the placebo group. Similarly, there was no difference between groups on low birth weight LBW30. Thus routine zinc supplementation in pregnancy is not advocated. In zinc deficient women, it may be of use.
Selenium Selenium is important in the role of glutathione peroxidase pathway to remove damaged cellular peroxidases, hence antioxidant activity. Serum selenium concentrations are reduced in women with preeclampsia compared with normotensive pregnant controls. A group from Beijing randomized 52 women at high risk for developing preeclampsia to receive 1000 µg per day of liquid selenium or placebo for 6 to 8 weeks during late gestation. There was a decreased incidence of pregnancy-induced hypertension from 22.7% to 7.7% in the treatment group.
Male infertility: Scott et al concluded in a double blind placebo controlled study that men with low sperm motility could improve their sperm motility with selenium in the dose of 100umg/day or selenium with vitaminA1mg, with vitaminC10mg with vitaminD15mg for 3 months. Thus selenium, in the dose of 1000umg/day in pregnant women at high risk for preeclampsia and in the dose of 100umg in male infertility could be useful . There are no studies on whether incorporating selenium in smaller doses in multivitamin tablets will achieve the same effect.
Fatty acids
Omega-3 fatty acids Omega-3 fatty acids are essential polyunsaturated fatty acids (PUFA) necessary for human health, but are not made by the body and hence must be obtained from a person’s food. Docasohexanoic acid and Ecisopentanoic acid are two types of Omega-3 fatty acids. Omega-3 fatty acids are found primarily in cold-water fish (salmon, herring, and mackerel) and several nuts and seeds.
These essential fatty acids and their metabolites are important in cervical maturation, parturition, initiation of labour, rupture of membranes, and birth. If there are low levels of omega-3 fatty acids and high levels of omega-6 fatty acids, there is an increased incidence of inflammatory prostaglandins, which are associated with preterm labor and intrauterine growth retardation32. Three randomized placebo-controlled clinical trials supplemented with either 920 mg of DHA and 1.3 g of EPA per day (total n-3 fatty acid intake of 2.7 g per day) or DHA-enriched eggs (205 mg of DHA per day without any EPA), found fewer low-birth-weight infants (LBW), preterm infants, and, in the trial using eggs, fewer women with gestational diabetes.
Supplementation with Omega 3 fatty acids in pregnancy has also been shown to increase IQ and visual acuity in the offspring in a few studies. It is a moot point whether higher IQ is directly proportional to increased productivity in life. This is an era where emotional quotient is considered as important as intelligence quotient for success in life. Thus it has to be debated whether all pregnant women should routinely be supplemented with omega 3 fatty acids. In light of the placebo controlled studies using 920 mg of DHA and 1.3 g of EPA per day finding lower incidence of preeclampsia and low birth weight babies, omega 3 fatty acids could be used in susceptible women towards this end. However most organizations recommend 200-300 mg DHA and EPA per day.
Amino acids
Arginine Arginine is an essential amino acid and plays an important role in cell division, the healing of wounds, removing ammonia from the body, inimmune function, and the release of hormones. It is the immediate precursor of nitric oxide. It has been found to improve uteroplacental blood flow because of its vasodilating effect.
Preeclampsia and IUGR:
Sieroszewski and colleagues in an ultrasound evaluation of the efficacy of L-arginine as a therapy for growth retardation found that the group treated with L-arginine 3g daily orally for 20 days had only 29% women with retarded babies as compared to 73% in the untreated group.
Some investigators have proposed the use of the nitric oxide test to identify pregnancies with Foetal growth restriction. The test consists of giving the mother 0.3 mg of glyceryl nitrate sublingually and then evaluating the uterine artery by Doppler velocimetry. Positive tests would select women who may benefit from treatment with nitric oxide donor agents like Arginine.
The average Indian practitioner may desist from performing too many tests on a patient and may benefit from supplementing a woman with Arginine in indicated cases where there is a bad obstetric history,uterine artery notching at 20 weeks or oligohydramnios and features of IUGR, etc. It is available in 3gm satchets. If it is given all at once in the day it can cause nausea. It should be given in 3 divided doses. Some patients find it difficult to tolerate even in divided doses.
Infertility: Arginine by it’s’ vasodilating effect was found to improve endometrial flow and thereby increase the successful rate of implantation of embryos in ART cycles. Battaglia et al concluded that oral L-arginine supplementation in poor responder patients may improve ovarian response, endometrial receptivity and pregnancy rate28.
However, in a later study,Battaglia et al evaluating the role of L-arginine supplementation in controlled ovarian hyper stimulation, concluded that Arginine supplementation may be detrimental to embryo quality and pregnancy rate during controlled ovarian hyper stimulation cycles. In this study , arginine was used in very high doses (8gm/day) and we do not know if it is this high dose which caused the detrimental effect.
Arginine is found in chocolate, wheat germ and flour, buckwheat, granola, oatmeal, dairy products (cottage cheese (Paneer), ricotta, nonfat dry milk, skim yogurt), beef , pork , nuts (coconut, pecans, cashews, walnuts, almonds, Brazil nuts, hazel nuts, peanuts), seeds (pumpkin, sesame, sunflower), poultry, seafood (halibut, lobster, salmon, shrimp, snails, tuna in water), chick peas, and cooked soybeans.
Carnitine
Carnitine, also known as L-carnitine (levocarnitine) is a quaternary ammonium compound synthesized from the amino acids lysine and methionine and is responsible for the transport of fatty acids from the cytosol into the mitochondria. It has been speculated that during growth or pregnancy the requirement of carnitine could exceed its natural production. The major sources of carnitine in the human diet are meat, fish and dairy products.
In male infertility: L-Carnitine (LC) and acetyl-L-carnitine (ALC) are highly concentrated in the epididymis and play a crucial role in sperm metabolism and maturation. They are related to sperm motility and have antioxidant properties. Carnitine enhances sperm energy production and, therefore, motility. Carnitine also has an antioxidant capacity and it protects sperms from oxidative damage Garella et al in a study concluded that in the presence of normal mitochondrial function(patients with normal phospholipid hydroperoxide glutathione peroxidase (PHGPx) levels), carnitine, in the dose of 2 gm per day for 3 months improved sperm motility. Vicari et al proved that in patients with prostate-vesiculo-epididymitis, treatment with 1gm carnitine and 0.5gm acetyle carnitine twice a day increased sperm forward motility and viability. Treatment with carnitine in these patients would have better effect if they were pretreated with anti-inflammatory agents.
However, when Sigman et al randomly selected a group of men with idiopathic oligoasthenospermia, and treated a group with carnitine 2gm/day and acetyle carnitine 1gm/day for 24 weeks, the motility and count did not significantly improve as compared to the group he treated with placeboes29. In a multicenter study of 100 patients treated with 3 gm carnitine for 4 months significant improvement in sperm motility was reported by Lewin et al, particularly in patients with idiopathic asthenospermia.14
Enzymes
Coenzyme Q10
Coenzyme Q(10) (CoQ(10)) is the predominant form of ubiquinone in man. CoQ(10) functions as an electron carrier in the mitochondrial respiratory chain as well as serving as an important intracellular antioxidant. Balercia et al in an open uncontrolled study found that Coenzyme Q10 in the dose of 200mg twice a/day for 6 months improved men with defective sperm motility23. This is probably the result of its role in mitochondrial bioenergetics and its antioxidant properties.
Coenzyme Q7, an analogue of Coenzyme Q10 was shown in the year 1967 to improve sperm motility significantly as reported by Tanimura J in Bull Osaka medical school journal . 35 years later, the only randomized controlled study on Co-enzyme Q10 comes from Balercia et al who used Co-enzyme Q10 in the dose of 200mg twice daily for 6 months in patients with sperm count >20mill/ml with forward motility less 50%. Coenzyme Q10 is used in the dose of 20-50mg for other indications, e.g.: cardiovascular indications.
In India, many pharmaceutical companies market this drug in the dose of 30-50 mg /day for asthenospermia. We still do not know if it is of any use, especially in this dose , for the majority of male patients who come to the infertility clinic, with the diagnosis of oligoasthenospermia, where both count and motility are affected.
Glutathione
Glutathione (L--glutamyl-L-cysteinylglycine; GSH) is the most abundant non-protein thiol in mammalian cells. It plays a key role in many biological processes, including the synthesis of proteins and DNA and the transport of amino acids, but notably, it plays a key role in protecting cells against oxidation: the sulphydryl (SH) group is a strong nucleophile, and confers protection against damage by oxidants, electrophiles and free radicals . Parenteral glutathione in the dose of 600mg IM on alternate days for a period of 2 months in a study by Lenzi et al resulted in significant improvements in overall motility, progressive motility, velocity, linearity, amplitude of lateral head displacement and beat cross frequency, together with a significant reduction in the proportion of forms with abnormal morphology. Although the magnitude of the improvements was not large, the increases in velocity, for example, were apparent within 30 days of starting treatment, and persisted for some time after the cessation of treatment, suggesting effects both on epididymal spermatozoa and on the seminiferous epithelium.
Carotenoids
Lycopene Lycopene is a dietary carotenoid with a potent antioxidant activity. It quenches singlet oxygen and scavenges peroxyl radicals. In preeclampsia: Sharma et al conducted a prospective clinical trial which randomized 251 primigravida women to receive oral lycopene (2 mg twice daily beginning at 16-20 wks) or matched placebo. Women randomized to lycopene were less likely to develop preeclampsia (8.6% vs. 17.7%, P < 0.05) than those who received placebo.
In Male infertility:Palan and Naz measured seminal lycopene by high pressure liquid chromatography in 37 men and noted significantly lower lycopene in the seminal plasma of immuno-infertile men than in fertile men. Gupta and Kumar treated 30 infertile men with 4 mg lycopene for 3 months and found a significant improvement in sperm counts and motility with no significant changes in sperm morphology. A 20% pregnancy rate was seen during the course of the study.
Folic acid and Vitamin B6 Steegers-Theunissen et al and Wouters et al found an association between hyperhomocysteneimia and embryo toxicity, leading to neural tube defects or spontaneous abortion, or vascular toxicity, leading to placental infarcts or abruption placentae. Hyperhomocysteinemia during pregnancy is also risk factor for both development of preeclampsia and its complications Hyperhomocysteinemia can be corrected, with a combination of folic acid and vitamin B6.
Leeda et al studied 207 patients with PIH or IUGR and found 37 them to have hyperhomocysteinemia and were given folic acid 5mg and vitaminB6 250 mg supplementation. 14 of them became pregnant while on treatment and had improved pregnancy outcome in their subsequent pregnancy, thus encouraging the use of these agents in hyperhomocysteinemic patients to prevent adverse effects of preecclampsia and IUGR. The average Indian practitioner would rather give empiric treatment with folic acid 5mg and vitamin B6 250mg for all patients with history of pre-eclampsia and IUGR than let all of them undergo tests to detect hyperhomocysteinemia. For the academically inclined, hyperhomocysteinemia can be detected by doing the methionine loading test.
Vitamin B12
A series of articles in the Japanese journal Hinyokika koyo published between 1984 and 1988 have found methylecobalamin in the dose of 1500mg/day to be useful in increasing sperm concentration. Isoyama et al in 1986 in a study studied the effect of Methylcobalamin CH3-B12 + Clomid (CH3-B12: 1,500 micrograms/day, daily and Clomid: 25 mg/day for 25 days followed by a 5-day rest period, for 12 to 24 weeks in men with counts above 10million/ml and found that sperm counts increased significantly in this population of patients compared to methylcobalamin alone or clomiphene citrate alone.
Hyperhomocysteinemia could be managed with folic acid alone or with the addition of vitaminB6. If vitamin B12 is useful for this purpose, the exact dose is not known.
Miscellaneous
Phytoestrogens
Phytoestrogens are molecules with estrogenic activity that are found in plants: ‘phyto’ = plant; ‘estrogen’ comes from ‘estrus’ (period of fertility for female mammals; derived from the name of an ancient Anglo-Saxon fertility goddess, Oestre) + ‘gen,’ to initiate, generate. Three major types of known phytoestrogens are coumestans, isoflavones, and lignans .
Phytoestrogen supplements containing isoflavones derived mostly from soya are very popular as an alternative therapy for menopause in India. Isoflavonoids are phytoestrogens present in soybeans concomitantly with soy protein, and they structurally and functionally resemble estradiol. Consumption of as little as 30 mg soy isoflavones, in soy protein or as an extract, reduces vasomotor menopausal symptoms by 30–50%. Isoflavonoids may reduce ghrelin levels and thus hunger and weight;(ghrelin is a recently detected hormone synthesized in the stomach in response to insulin-induced hypoglycemia and is capable of increasing appetite by stimulating hunger).There are no effects of isolated isoflavonoids(114mg) on lipids, lipoproteins, or insulin sensitivity in postmenopausal women, implying no vascular benefit. It also has no proven benefit on genitourinary symptoms, or osteoporosis.
Breast cancer is a common concern while using standard estrogens, and isoflavones are thought to be an attractive alternative to them, particularly in breast cancer survivors, and in those women at high risk for breast cancer. In a double blind study of breast cancer survivors, by Mc Gregor et al, there was no difference in menopausal symptoms in breast cancer survivors, between two groups, one taking placebo and the other soy supplements. However, in Asian countries, where soy is being used since childhood in diet, it does seem to offer some sort of decrease in breast cancer rate. This effect possibly cannot be emulated by concentrated soy supplements used for a short time later in life as in clinical trials.
Practitioners using soy suppliments would do well to give realistic expectations to their menopausal patients. It may decrease hot flushes to some extent, though not as effectively as traditional HRT. Its other benefits for menopausal patients other than hot flushes remain controversial. Again, cancer prevention going by the decreased cancer incidence in the soy consuming nations, may not work out too well in populations who start these suppliments late in life for short periods of life.
Conclusion:
Research in new molecules usually requires a lot of stringent studies and they can be available for clinical use only after they have been approved by drug controllers. However, nutritional supplements need not always need these approvals before they are available for use; hence the widely prevalent use of these substances in clinical practice for indications, for which there are still no remarkable breakthroughs by way of therapy.
The presence of several mechanisms to counteract oxidative stress leads to the need for multiple antioxidants as defence against reactive oxygen species radicals. Antioxidants should be used in correct dose to achieve desired results. Overdose should be avoided as in high doses it may decrease the level of free oxygen radicals to less than what is needed for physiological functions.
These drugs used judiciously, could be a boon to many patients with bad obstetric history, male infertility and unexplained infertility.
Side Effects Of Oral Contraceptives
Posted On April 26, 2018 by Dr.Shobhana Mohandas
Oral contraceptives are widely used world over, but it’s use in India is comparitively less, due to fear of side effects. Following is a brief account of side effects of oral contraceptives.
Major side effects
- Increased incidence of CVS diseases, viz venous thromboembolism, heart attack including ischaemic heart disease, cerebrovascular disease or stroke and hypertension.
- Weak association between long term use of OC and breast cancer diagnosed before the age of 36.
- Reduced glucose tolerance
- Cholestasis
- Clotting disorders, Pulmonary embolism.
- Abnormal thyroid and adrenal function
- Changes in lipid and lipoprotein metabolism
Minor side effects
- Break through bleeding, amenorrhoea
- Breast tenderness or fullness
- Nausea
- Weight gain
- Headache
- Decreased libido
- Less commonly, dermatologic effects, like acne, gum inflammation, increased viral infections, cervical ectropion (which may increase the risk of chlamydia),
Oral contraceptives are least used in India, China and Japan. However, with increasing urbanization and change in life style, there is an increased demand for the pill in India also. With newer molecules being marketed to avoid the side effects produced by older preparations, it is necessary to remain appraised of the side effects caused by “pill” as well as the effects it may have on various medical conditions.
To enumerate in short, the side effects caused by oral contraceptive pils(OC’s) could be major or minor, and they are listed in the table below.
Women may not accept OC as a method of contraception as they are afraid of side effects, but seldom abandon the use of OC’s due to side effects per se. Lacks of accessibility, failure to take the drug regularly, etc are more common reasons for discontinuation. The most common treatment-related adverse effects are headache, nausea, breast tenderness, and weight gain.
Nausea,bloating : Found occasionally in a few patients, it is usually not very bothersome. Low fat,low residue, spaced meals, reduce functional nausea. In addition, changing the OC to a high progesterone, low estrogen combination could be tried. The symptoms of bloating or swelling begins in the active week before the hormone-free interval and is most prevalent during that time3.
Break through bleeding: Breakthrough bleeding is greatest in the first 3 months and it’s frequency decreases after that. Low dose oestrogen pills containing 20 microgram of estrogen are more likely to produce disorders in cycle control. It is even more frequent in women taking COC 15-μg Ethinyle Estradiol (EE) than in those using 20-μg EE. Pills containing norethisterone produce more irregularities than those containing levonorgestrel.
If the woman could be reassured that bleeding will not reduce contraceptive efficacy and that it is only the result of the endometrium trying to adjust it’s thickness to the new hormone levels, no treatment need be given. However, if it is distressing, to continue to let the woman enjoy the benefits of low dose oestrogen pills, these women could beneficially be given 1.25mg conjugated estrogen or 2 mg estradiol daily for 7 days when bleeding is present. If 1 course of oestrogen is not enough, another 7 days of estrogen use is effective.
Amenorrhoea: Amenorroea is an uncommon side effect found in some women, caused by endometrial atrophy. It is distressing to some women, as it may be a sign of unwanted pregnancy. Addition of extra oestrogen for 1 month (1.25mg conjugated oestrogen or 2mg estradiol) daily throughout the 21 days of that cycle will rejuvenate the endometrium and withdrawal bleeding resumes, persisting for many months. This could be resorted to in patients who prefer not to remain amenorrhoeic.
Headache: Headache, specially, migrainous headache is more prevalent in OC users. Migrainous headaches frequently occur in the hormone free period, when oestrogen levels are falling. Use of estrogen replacement in this hormone free period could reduce this symptom. However, women with migraine accompanied by aura are best advised to avoid OC’s. Evidence from six case-control studies suggested that COC users with a history of migraine are four times as likely to have an ischemic stroke as nonusers with a history of migraine.
Weight gain: Weight gain due to water logging caused by progestin content was a common complaint in the past. The current low-dose OC containing 20 μg ethinyl estradiol EE and 100 μg LevononorgestrelLNG did not cause weight gain and was safe and well tolerated in a double blinded placebo controlled trial. In another trial, among users of two 20mcg oestrogen-containing pills, in a one-year trial, 13% lost >2kg, 74% stayed at the same weight+2 Kg, and 13% did gain >2kg. In fact, studies have shown that women often begin taking the pill during a time of life that typically coincides with weight changes, giving the pill an undeserved reputation for adding weight.
Breast tenderness: Incidence of this complaint is less with use of low dose estrogen pills. In a study comparing 3 types of contraceptives, participants in the Levonogestrel containing OC pill group experienced nausea, breast tenderness and irritability more frequently than did those in the other groups, using gestodene and etonogestrel as progestins. Shortening the hormone-free interval from 7 to 4 or 5 days might increase the contraceptive safety margin and decrease the prevalence of symptoms such as breast tenderness and headaches.
Major side effects: Combined oral contraceptives are by and large very safe. However, in the rare special cases, it may cause serious side effects and awareness of these side effects could prevent major complications in these special category patients.
Cardiovascular side effects: A WHO study found no increased risk of heart attack among healthy pill users.
Less than 5% of women using hormonal contraception develop hypertension, which may increase their risk for heart attack and stroke1. Blood pressure checking should be an important part of clinical evaluation of pill users.
Thrombotic events: Oral contraceptives (OC) have been implicated in causing increased blood coagulation. The hormone changes during pill ingestion are akin to those occurring in pregnancy and similarly, the risk of thrombotic events is also present only in the rare individual prone to it. The risk posed is actually less than that incurred by pregnancy. Women with an inherited resistance to activated protein C, the factor V Leiden mutation, congenital deficiencies in antithrombin III, protein C, or protein S, are prone to thrombotic events.
Acute maculo-neuroretinopathy, macular haemorrhage, central retinal vein occlusion, central retinal artery occlusion, and perivasculitis have been reported, mostly in patients on oral pills for a long time. Although long term use is unlikely in India, a rare case of central retinal artery occlusion following OC pills has been reported from India after 4 months of use of Mala-D2.
The risk of development of deep vein thrombosis was also found to be 2 to 5 times greater with a low-estrogen, desogestrel-containing oral contraceptive than with second-generation monophasic and triphasic preparations(containing progestin of the norgestrel type). Because desogestrel may have benefit for some patients, specially women with excessive androgen activity, one may restrict its use only for selected users prone to such thrombotic events.
Risk of cancerOral contraceptive use is associated with a very slight increase in breast cancer risk (relative risk=1.2) for current users vs. never-users. However, breast cancer risk associated with the use of oral contraceptives disappears with time when use is discontinued. 1-4 years after discontinuation the relative risk is 1.16, at 5 to 9 years after use the risk is 1.07, and by 10 years from last use, breast cancer risk of ever-users is not different from never-users. It has been found that even in women with familial cancer syndrome, incidence of breast cancer is not higher among oral contraceptive users compared to non-users.
There is an increased incidence of cervical cancer in HPV positive women on prolonged use of oral contraceptives (>5 years). Till HPV screening becomes cheap and routine, yearly pap smear should be recommended for all women on oral contraceptive pills.
Incidence of ovarian cancer is reduced in OC users and incidence of colorectal cancer is reduced in current users of OCs. There is no increased incidence of hepatocellular cancer and effect on lung cancer is known with use of OC’s. Glucose intolerance: increased insulin resistance in pill users is generally met by increasing insulin secretion, and there is just a slight elevation of 1 hour glucose levels. Low dose pills may be used by diabetic women. However, high, pharmacologic dose of estrogen should be avoided by women with diabetes and vascular disease or major cardiovascular risk factors.
Oral contraceptives and medical problems:
Women who should avoid combined oral contraceptive pills:
- Women known to have stones or a positive history for gallbladder disease.
- Women with triglyceride levels >20mgm/dl and women with existing vascular disease.
- Mitral valve prolapse complicated with atrial fibrillation, migraine headaches, or clotting factor abnormalities .
- Women with congenital heart disease or valvular heart disease if there is marginal cardiac reserve or a condition that predisposes to thrombosis.
- Smokers over 35 years of age
- Women with systemic lupus erythematosus.
Conditions where combined oral contraceptives are safe:
- Women younger than 35 years who have hypertension well controlled by medication and who are otherwise healthy and do not smoke.
- Women with pregnancy induced hypertension after the Blood pressure is normal
- Women with history of gestational diabetes.
- Women with fibroids, if low dose pills are used.
- Benign breast disease.
- Women with seizure disorders. However, some antiepileptic drugs decrease efficacy of the pill, and this should be kept in mind.
- Women with depression.
- Women with sickle cell trait.
- Women with hemorrhagic disorders and women taking anticoagulants.
- Infectious mononucleosis provided liver function tests are normal.
- Ulcerative colitis
- Regional enteritis (Crohn’s disease).
- Elective surgery if prolonged immobilization is not anticipated and if low dose preparations are used. COC should be used till the last day before sterilization operation is performed if the woman is using it as a contraceptive measure.
- Women with varicose veins, provided it is not very extensive.
Conclusion:
The newer low oestrogen contraceptives and the use of newer progestins accompanying it have reduced side effects of combined oral contraceptives to a great extent. Most of the studies which showed side-effects of oral contraceptives were done on the earlier preparations with high oestrogen content. However, while using oral contraceptives for dysfunctional uterine bleeding, higher oestrogen doses may have to be employed and in these patients, the practitioner should be aware of all side effects, to take effective steps.
Ectopic pregnancy Pitfalls In Management
Posted On April 25, 2018 by Dr.Shobhana Mohandas
Management of Ectopic pregnancy entails some special situations, which are discussed below with illustrative examples.
Medical management without drugs:
- Ectopic management can be managed expectantly in woman with an initial hCG level of less 1000IU/l.
- They should be haemodynamically stable, should not have abdominal pain ,
- USG should not show peritoneal fluid greater than 100ml, and there should be no adnexal mass > 2cm.
- This situation is usually not so common, as one does think of Ectopic pregnancy only when the patient has some sort of pain.
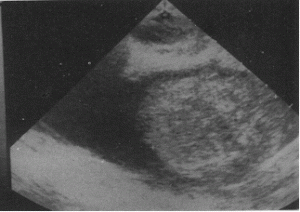
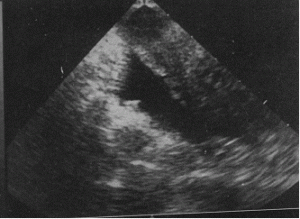
The first picture shows fluid in the cul-de-sac in ectopic pregnancy, while the second picture shows fluid in the cul de sac in normal ovulation; Thus ,it is plain that fluid in cul-de-sac should not be an indication to press the panic button. This is because, fluid in cul-de-sac could be seen in normal ovulation and sometimes in pelivic infection. However, if the fluid is greater than 100ml, expectant management is not recommeneded. Expectant management requires measurement of hCG levels twice weekly for the first two weeks and thereafter weekly until it’s disappearance. there is a reported failure rate of only 4-6% with expectant management in such patients. this situation would, logically arise in infertility patients where early scans are performed more often.
Early Pregnancy loss: Early pregnancy loss is quite often associated with abdominal cramps. Sometimes, other pelvic causes for pain may occur concomitantly, confusing the picture. This is why, in cases with no intra-uterine gestational sac and a positive pregnancy test, one should not jump to a conclusion of ectopic pregnancy and should desist from aggressive treatment with Methotrexate. The falling hCG levels seen in early pregnancy loss is in contrast with the slow rise of hCG titres found in live ectopic pregnancy.
Case history 1 A 40 year old lady with 4 children came with history of lower abdominal pain, bleeding PV, 2 weeks delayed periods and a positive pregnancy test. Intrauterine cavity failed to show a gestational sac on the initial ultrasonography and the patient had stones in the right ureter. The character of pains that she described was however not typical of stone. The doctor tested the serum for 2 values of hCG which showed 7500 and 3500 respectively, indicating that she had a pregnancy which was gradually, losing it’s viability, whether it be in the uterus or the tube. Severe tenderness on attempting TVS percluded a proper assessment of the endometrial cavity and she was referred to me. After reassurance, and medical management for urolithiasis, a repeat ultrasonography was done, this time with a high resolution 3D/4D machine. TVS now showed some products in the cavity. The products were evacuated. This underlines the need to do 2 hCG values as was correctly done in this case, before making a diagnosis of ectopic pregnancy.
Case history 2 A 30 year old G2 P2 with H/O 2 previous LSCS and tubal ligation, came with history of 10 days amenorrhoea and mild abdominal pain. Ultrasonography in a portable machine did not show a sac in the uterus or outside. An ectopic pregnancy was diagnosed. Ideally, even if there is a sac, if the size is less than 2cm, the patient could be a candidate for Methotrexate. This patient had lost her faith in ligation as a method of contraception and just wanted cure of ectopic pregnancy. I did not wait for 2 values of hCG. A baseline value of hCG was taken and inj.Methotrexate50mg given IM in the evening . The pictures below were taken next day morning and show how the ectopic was extruded out. USG taken 2 days later showed resolution of the fluid and the patient remained asymptomatic thereafter. Thus, even if fluid is seen in the pouch of douglas after injection of methotrexate, if it is not of a large amount, one need not worry.
USG taken 2 days later showed resolution of the fluid and the patient remained asymptomatic thereafter. Thus, even if fluid is seen in the pouch of douglas after injection of methotrexate, if it is not of a large amount, one need not worry.
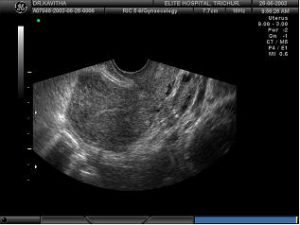
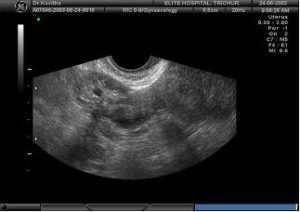
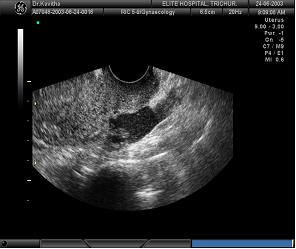

- 9 AM Slight fluid in POD.
- 9.06AM quantity increased.
- 9.09AM increasing fluid
- 2 days later: Fluid has disappeared
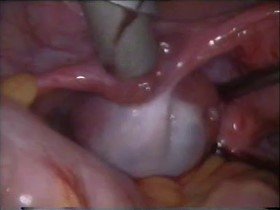
case 3: A patient with missed periods with serum beta hcg showing 50 units came with acute abdominal pain. Ultrasonography showed lot of fluid ?blood in pelvis with a mass in left adnexa.Left ovary is enlarged and uterus is empty.Laparoscopy was done to rule out ruptured ectopic, though patient was haematologically and otherwise stable.
Misoprostol In 1stand 2nd Trimester
Posted On April 28, 2018 by Dr.Shobhana Mohandas
- Misoprostol In 1stand 2nd Trimester
Ovarain Cyst
Posted On April 6, 2018 by Dr.Shobhana Mohandas
Ovarian cysts are quite often functional cystic spaces in the ovary. But sometimes they could be endometriomas or if there are solid areas present, may harbour malignancy. Current management principles of ovarian cysts are outlined below:
Asymptomatic unilateral cysts in the adolescent:
Unilateral ovarian cysts in the adolesent with pain: If the patient has persistent pain accompanied by autonomic symptoms like vomiting, one has to think in terms of a twist in the ovarian cyst. Identification of the twisted vascular pedicle through ultrasonography is suggestive of ovarian torsion, and color Doppler sonography could be helpful in predicting the viability of adnexal structures by depicting blood flow within the twisted vascular pedicle. A diagnosis of twisted ovarian cyst warrants surgery. During surgery, a bluish colour in the cyst on initial inspection is not confirmatory of gangrene in the ovary. In some cases, untwisting of the cyst may bring back vascularity to the ovary, which may then regain its original colour (8). A cystectomy may now be done. In case the ovary has undergone gangrene, adnexectomy is the only option. Laparoscopic techniques if available are kindest to the patient in these circumstances. If the patient has symptoms of endometriosis like congestive dysmenorrhoea, an endometrioma has to be suspected. In India, Ultrasonography in this age group is usually done with transabdominal probes, which may be inadequate to distinguish a simple cyst from an endometrioma. Endometriomas should be managed by laparoscopic ovarian cystectomy and coagulation of any other endometriotic implants.
Unilateral unilocular simple ovarian cyst in the reproductive age group: In this age group, a vaginal sonography is possible, and in expert hands, a differentiation can be be made between a simple cyst and an endometrioma, the latter showing internal echoes. A simple cyst could be observed for 3 months. If it does not disappear, the diagnosis of a benign ovarian neoplasm like serous or mucinous cystadenoma should be made. If the patient has completed her family, salpingo-oophorectomy could be done on the affected side, instead of cystectomy. Hysterectomy is a much more complicated procedure compared to ovarian cystectomy and is not warranted for treatment of benign neoplastic cysts. Endometriomas in this age group should be tackled taking in to consideration the findings in the rest of the abdomen. If there is extensive endometriosis in the pelvis, it may be prudent to do a hysterectomy with bilateral oophorectomy if the patient has completed her family. She should subsequently be put on hormone replacement therapy to prevent symptoms of oestrogen deficiency.
Ovarian cysts with solid areas in the adolescent age group: The presence of solid areas in the cyst makes the mass a complex mass. Complex masses should alert one to the possibility of neoplasms, benign or malignant. However, the mere presence of solid areas is not diagnostic of neoplasm. Complex cysts could be corpus luteum cyst, hemorrhagic cyst, ectopic pregnancy, ovarian torsion, tubo-ovarian abscess or appendiceal abscess,
endometrioma, or either benign or malignant neoplasm. Assuming that pregnancy, torsion, and infectious causes are excluded, a repeat sonogram should be performed after the next menses. Patients with pain may need to be scanned at a shorter interval. Hemorrhagic cysts can have a variable sonographic appearance that commonly changes over a period of days. If the mass decreases in size on ultrasound follow-up, it can continued to be followed. If the cyst persists for longer than two or three cycles, then neoplasm is more likely, and surgical evaluation is indicated. As with simple cysts, increase in size, pain, or mass effect should prompt earlier surgical intervention. Malignancy should be suspected on ultrasonography in some cases by observing the thickness of the capsule, shadowing, echogenecity, etc. Even if the ovarian cyst is palpable over the umbilicus, In the author’s experience, if an ovarian cyst is palpable above the umbilicus, unilocular and filled with clear fluid as shown on Ultrasound, it is possible to select a site on the abdomen where the cyst is looking tense and adjacent to the abdominal wall and put a needle in and aspirate the fluid through suction. Now it becomes easier to put in the laparoscope and salpingooophorectomy/cystectomy becomes possible. In a large cyst, the thinner portion of the cyst is first excised. This makes it easier to delineate the ovarian wall from the cyst wall. A cystectomy can now be performed. However, in a huge ovarian cyst, the functional ovarian tissue left behind after such a procedure is very less.
Unilateral cysts in the menopausal woman: If the cyst is only 3-5cm, she should have a serum CA-125 level done and a color doppler sonography done. If CA–125 levels are less than 65IU and colour doppler is suggestive of a nonmalignant lesion, she could be followed up at 2,3,6,9, and 12 months and annually there after. In cysts larger than this a unilateral salpingo-oophorectomy should be done, provided the CA125 levels and color doppler is suggestive of a nonmalignant lesion. An international multicenter study found that postmenopausal patients with an asymptomatic simple ovarian cyst 3-5 cm in diameter and a normal CA125 had a 0% risk of malignancy (6). CA125 is an antigenic determinant that is elevated in 80% of all patients with serous cystadenocarcinoma of the ovary but in only 50% of the patients with stage I disease. As a diagnostic aid, measurement of CA125 is most useful in postmenopausal patients with an ultrasonographically suspicious mass. In this setting, a level greater than 65 U/mL has been shown to have a positive predictive value of 97%. Color flow Doppler has been reported to be helpful in identifying malignancy. Computerized tomography (CT) does not have as good resolution of ovarian masses as ultrasound but does tell you a lot about the rest of the abdomen. Magnetic resonance imaging (MRI) is a little better at describing ovarian masses and, like CT, gives a good view of the entire abdomen; however, MRI is more costly. In summary, simple unilocular cysts are likely to be benign but should always be followed up with Ca- 125 levels. If it is greater than 65 U/ml, to be on the safe side the patient should be treated as ovarian malignancy. When CA125 levels are normal, the patients should be followed up.
Multilocular cysts: Multilocular cysts as opposed to simple cysts need careful evaluation. Cysts >6cm should alert one to the possibility of malignancy. The differential diagnosis of such a cyst in this age group should include an inflammatory tubo-ovarian mass, an endometrioma, a benign Teratoma (Dermoid) or even a hemorrhagic corpus luteum cyst.. In all these conditions a laparoscopic cystectomy/salpingo-oophorectomy is all that is needed. Here, it is useful to remember that CA-125 is elevated (>35mIU) in endometriomas, Pelvic infections, pregnancy and assossiated liver disease. A markedly elevated Ca-125 (>200mIU) may make one strongly suspect malignancy and take a decision straight away in favour of a hysterectomy with bilateral salpingo-oophorectomy. A normal CA-125 level alone is not enough to rule out malignancy. Quite often the diagnosis of borderline malignant ovarian tumour is made presumptively at the time of surgery on seeing the excrescences on the tumour, adhesions etc, confirmation being made only after histopathology. Thus in a patient with multilocular cysts, a colour doppler scanning and testing of serum for tumour markers might help in preoperatively detecting malignancy, but even if preoperative evaluation does not indicate malignancy a careful histopathology is mandatory postoperatively.
Ovarian cyst in pregnancy: Traditionally, asymptomatic ovarian cysts >8cm should be removed only after 16 weeks as till then there is a possibility that the cyst is a corpus luteum cyst. Asymptomatic corpus luteal cysts disappear in second trimester. But symptomatic cysts (Torsion, haemmorrhage, rupture) should be removed even in first trimester.Ultrasonographic cyst aspiration could be tried in selected cases.(20) In cases where cystectomy is done before 10 weeks, progesterone support should be given as the corpus luteum may have been removed.Progesterone suppositories are available in strengths of 100mg and 200mg. These could be given twice daily orally or vaginally. Vaginal route is known to give better absorption rates. One study has reported 6 cases of laparoscopic cystectomy for adnexal torsion without miscarriages, proving that in skilled hands laparoscopy is safe in 1sttrimester(17). The author also has done 2 laparoscopic ovarian cystectomies in first trimester of pregnancy with good maternal and fetal outcome. Ovarian cysts getting impacted in the pouch of Douglas causing obstruction to labour in second stage could also be aspirated.
Myomectomy in infertile women: The impact of leiomyomata on reproduction is not clear due to the paucity of well controlled studies.(15). Intracavitary and large submucosal leiomyomata are most likely causally related to infertility. . Removal of submucosal and large intramural leiomyomata has been associated with improved outcome in infertile women undergoing assisted reproductive technologies such as in vitro fertilization(8). If the clinical problem is repeated miscarriage,preterm labor, or intrauterine growth restriction or the leiomyomata are large,preconceptional removal of intramural leiomyomata may be appropriate. All patients with myomas should be educated about specific risks during pregnancy, including miscarriage, pelvic pain,premature labor, and postpartum hemorrhage. In the absence of other causes of infertility or after the unsuccessful treatment of other infertility factors, it is reasonable to suggest myomectomy as an option. Most patients can be treated without surgery. There is ultrasonographic evidence of recurrence in 25% to 51% of patients, and as many as 10% require a second major operative procedure (9). According to one study(29), most recurrences occur10-30 months following original surgery. Myomectomy removes only the fibroids, the genetic predisposition for the formation of fibroids remaining intact.
Q: What should be management of a unilocular simple 3-5 cm cyst in a menopausal woman? A: The possibility of malignancy has to be kept in mind, more in the postmenopausal woman. The protocol of management should be the same. An international multicenter study found that postmenopausal patients with an asymptomatic simple ovarian cyst 3-5 cm in diameter and a normal CA125 had a 0% risk of malignancy3. CA125 is an antigenic determinant that is elevated in 80% of all patients with serous cystadenocarcinoma of the ovary but in only 50% of the patients with stage I disease. As a diagnostic aid, measurement of CA125 is most useful in postmenopausal patients with an ultrasonographically suspicious mass. In this setting, a level greater than 65 U/mL has been shown to have a positive predictive value of 97%. In RCOG guidelines2, It is recommended that ovarian cysts in postmenopausal women should be assessed using CA125 and transvaginal grey scale sonography. There is no routine role yet for Doppler, MRI, CT or PET.
Q: What should be the management of a multilocular cyst in the post menopausal woman” A: Multilocular cysts as opposed to simple cysts need careful evaluation. Cysts >6cm should alert one to the possibility of malignancy. The differential diagnosis of such a cyst in this age group should include an inflammatory tubo-ovarian mass, an endometrioma, a benign Teratoma (Dermoid) or even a hemorrhagic corpus luteum cyst.. In all these conditions a laparoscopic cystectomy/salpingo-oophorectomy is all that is needed. Here, it is useful to remember that CA-125 is elevated (>35mIU) in endometriomas, Pelvic infections, pregnancy and assossiated liver disease. A markedly elevated Ca-125 (>200mIU) may make one strongly suspect malignancy and take a decision straight away in favour of a hysterectomy with bilateral salpingo-oophorectomy. A normal CA-125 level alone is not enough to rule out malignancy. Quite often the diagnosis of borderline malignant ovarian tumour is made presumptively at the time of surgery on seeing the excrescences on the tumour, adhesions etc, confirmation being made only after histopathology. Thus in a patient with multilocular cysts, a colour doppler scanning and testing of serum for tumour markers might help in preoperatively detecting malignancy, but even if preoperative evaluation does not indicate malignancy a careful histopathology is mandatory postoperatively.
Q. What should be the management of a menopausal woman with an simple ovarian cyst of larger than 6cm? A:In a woman with an ovarian cyst larger than 5 cm differentiation should be made between organic and functional cysts. Normally formed follicles or corpus luteum in the ovary may sometimes undergo cystic transformation, leading to formation of follicular cysts or corpus leuteal cysts, which are functional cysts. . The majority of follicular cysts disappear spontaneously by either reabsorption of the cyst fluid or silent rupture within 4 to 8 weeks of initial diagnosis 4. Unless ultrasound features definitely indicate organic cyst, a presumptive diagnosis of functional ovarian cyst could be made and the patient watched over for 6 months. However, persistence of the cyst over 6 months means there is likelihood that the cyst is not functional, and that it needs surgical intervention. If the patient has acute or chronic pelvic pain, which could be attributable to the cyst, surgical treatment is warranted, even if the cyst appears to be functional.
In younger women, if there is no suspicion of malignancy, ovarian cystectomy with conservation of ovary could have been done. But in a post menopausal woman, unilateral salpingooophorectomy with removal of the tissue without possible spillage into the abdomen would be the ideal treatment of choice. Laparoscopic surgery being a less morbid procedure, for the patient, should be preferred if the centre has facilities for laparoscopy. In case of suspected malignancy, although there are many reports of laparoscopic surgery in advanced centres, by and large, laparotomy is considered to be the gold standard.
A point scale (0 to 4) was developed within each category, with the total points per evaluation varying from 0 to 12.
An ultrasound morphology index score less than 5 in a pre-menopausal woman is in keeping with a benign aetiology.
have found no significant change in uterine size or myoma volume over 6–12 months of follow-up in placebo arms . A nonrandomized study of women who had uterine size of R8 weeks and who chose hysterectomy or watchful waiting found that 77% of women choosing observation
In post-menopausal patients, a morphology index score ≥5 has a positive predictive value for malignancy of 0.45.
Malignancy indexing can also be helpful in diagnosing malignancy in a post menopausal woman.
Risk of Malignancy Index(RMI) = U ×M ×CA 125.
U=Ultrasound score.
M=3, a constant for menopausal women.
CA 125=value of CA 125.
- Moderate-risk RMI = 25 to 250; Risk of cancer is 20%;
- High-risk RMI = >250 Risk of cancer is 75%;
- Low-risk RMI = less than 25; Risk of cancer is less 3%
Q: What are the risk factors for ovarian cancer? A: Family history of ovarian cancer is associated with increased risk of ovarian cancer. Family history of epithelial cancers are specially associated with increased risk of ovarian cancer. There are genetic markers, which can predict whether such an individual is at an increased risk of developing ovarian cancer. The most studied gene associated with ovarian cancer is the BRCA1 gene. If relatives of patients who develop ovarian cancer are found to have this gene, they could undergo frequent surveillance for development of ovarian cancer. If such individuals have to undergo hysterectomy, they should undergo a prophylactic bilateral oophorectomy as well. Similarly there are quite a few other genes also which have been found to be present in increased frequency in women with ovarian cancer. But, without further studies to confirm their usefuleness, it has not been found necessary to genetically screen the population as a whole to see who is at increased risk of ovarian cancer. These studies are available in India,but are prohibitively costly.
Post-menopausal women with suspicious pelvic mass and:
- Elevated CA-125 level (>35 U/mL)
- Ascites
- A nodular or fixed pelvic mass
- Evidence of abdominal or distant metastasis
- A family history of 1 or more first-degree relatives with ovarian or breast cancer.
Pre-menopausal women with a suspicious pelvic mass and:
- Greatly elevated CA-125 level (> 200 U/mL)
- Evidence of abdominal or distant metastasis
- Ascites
- A family history of 1 or more first-degree relatives with ovarian or breast cancer.
Risk factors for ovarian cancer: Family history of ovarian cancer is associated with increased risk of ovarian cancer.Family history of epithelial cancers are specially associated with increased risk of ovarian cancer. There are genetic markers, which can predict whether such an individual is at an increased risk of developing ovarian cancer. The most studied gene associated with ovarian cancer is the BRCA1 gene. If relatives of patients who develop ovarian cancer are found to have this gene, they could undergo frequent surveillance for development of ovarian cancer. If such individuals have to undergo hysterectomy, they should undergo a prophylactic bilateral oophorectomy as well. Similarly there are quite a few other genes also which have been found to be present in increased frequency in women with ovarian cancer. But, without further studies to confirm their usefuleness, it has not been found necessary to genetically screen the population as a whole to see who is at increased risk of ovarian cancer. These studies are as yet not available in India.
Infertility and nulliparity is associated with increased risk of ovarian cancer. The use of infertility drugs was suspected to increase the risk, but it has been found that it is infertility per se and not the use of ovulation inducing drugs that increases the risk of ovarian cancer.
Stage I Growth limited to the ovaries
- Stage IA Growth limited to one ovary; no ascites,No tumor on the external surfaces;capsules intact.
- Stage IB Growth limited to both ovaries; noascites. No tumor on the external surfaces;capsules intact.
- Stage IC Tumor either stage IA or IB, but with tumor on surface of one or both ovaries;or with capsule ruptured; or with ascitescontaining malignant cells; or with positive peritoneal washings.
- Stage II Growth involving one or both ovaries,with pelvic extension.
- Stage IIA Extension or metastases to the uterus or tubes.
- Stage IIB Extension to other pelvic tissues.
- Stage IIC * Tumor either IIA or IIB but on thesurface of one or both ovaries; or with capsule(s) ruptured;
- Or with ascitescontaining malignant cells; or withpositive peritoneal washings.
- Stage III Tumor involving one or both ovaries with peritoneal implants outside the pelvis or Positive retroperitoneal or inguinal nodes;
superficial liver metastasis equals stageIII;
tumor is limited to the true pelvis, but there is histologically proven malignant extension to small bowel or omentum - Stage IIIA Tumor grossly limited to the true pelviswith negative nodes but with Histologically confirmed microscopicseeding of abdominal peritoneal surfaces.
- Stage IIIB Tumor involving one or both ovaries with histologically confined implants of abdominal peritoneal surfaces, none exceeding 2 cm in diameter; nodes are negative
- Stage IV Growth involving one or both ovaries with distant metastases; if pleural effusion is present, there must be positive cytology to categorize as stage IV.
Benign tumours in adolescents: Breen and Maxson combined four series to demonstrate the shifting distribution of ovarian neoplasms by patient age. In young adolescents 10 to 14 years old, 72% of ovarian neoplasms were germ cell; 8%, sex cord stromal; and 16%,epithelial tumours. Among the older adolescents 15 to 17 years old, 49% were germ cell; 16%,sex cord stromal, and 28%, epithelial.
Cystic teratomas: Cystic teratomas (Dermoids) are the most common benign tumour in this age group. Dermoids are benign germ cell tumours. They usually contain skin, teeth, bones, hair, and extremities. . On sonography, dermoid cysts often appear as complex cystic masses that contain solid elements that cause shadowing. Laparoscopy or laparotomy can be used to remove dermoids by cystectomy in most patients or by oophorectomy when necessary. If the dermoid is larger than 6 cm or the patient has undergone multiple surgical procedures with adhesions, laparotomy is the preferred treatment approach.. Careful attention should be given to the other ovary because of the 12% rate for bilateral occurrence. There is a 1-2% chance of malignant change in Dermoids, but this is unusual in this age group, being an occurence seen usually in the post-menopausal age group.
Dysgerminoma: It is the commonest germcell malignancy.In early cases unilateral salingo-oophorectomy followed by surveillance is all that is necessary. In advanced cases, combination chemotherapy has to be added.
Other germ cell tumours: Other germ cell malignancies found in adolescents include immature teratoma, embryonal carcinoma, endodermal sinus tumor, gonadoblastoma, choriocarcinoma, and mixed germ cell tumors. Many of these tumors produce markers, as previously discussed, that may be useful for following response to therapy. Most patients should receive postoperative chemotherapy with bleomycin, etoposide, and cisplatin, with the exception of those with stage I, grade I immature teratoma, who can be followed with surveillance. The survival rate for these patients is not as good as those with dysgerminoma but is still excellent, especially for those with early stage disease with appropriate adjuvant chemotherapy.
Tumour markers in ovarian Ca in adolescent age group: Whenever a patient is suspected to have an ovarian malignancy, she should have the levels of tumour markers checked, both for diagnostic purposes and for following up the patient after surgery. The tumor marker, Cancer antigen 125(CA-125) is not as useful in adolescents as in menopausal patients. Elevation can be caused by a variety of processes that result in peritoneal irritation, such as endometriosis or PID, making the test nonspecific in this age group. Germ cell tumours are more common in this age group and the tumour markers specific to these tumours will be more useful in this age group.
Alpha-Fetoprotein can be made by endodermal sinus tumors, embryonal cell cancer, mixed germ cell malignancies, and rarely by immature teratomas. Serum beta-hCG can be found in nonpregnant patients with embryonal cell carcinoma and choriocarcinoma. Patients with dysgerminoma may have elevated lactate dehydrogenase levels. Tumor markers are most useful for following treatment response in patients diagnosed with ovarian malignancies.
Ovarian caner in the adult woman:
Epithelial tumours: Benign epithelial tumors: Conservative surgery with the preservation of some ovarian tissue is enough in young women with benign epithelial tumors. This usually includes ovarian cystectomy or oophorectomy. In postmenopausal women a TAH/BSO can be considered to avoid future cancer risk.
Malignant epithelial tumours: Almost 85% of all ovarian malignancies are derived from ovarian epithelium, making epithelial malignancies the most commonly encountered ovarian cancer. It could be borderline, or frankly malignant. They include, Serous, mucinous, endometrioid, clear cell, Brenner-transitional cell, mixed mesodermal, and undifferentiated tumors.
excrescences,rupturedcapsule,ascites,peritoneal implants,haemmorrhage and necrosis,solid areas or intracystic papillations. These tumours have to beremoved by cytoreductive surgery. Cytoreductive surgery is the removal of as much of the tumor and its metastases as possible. It includes TAH, BSO, and complete omentectomy with resection of any metastatic lesions. In some patients, bowel resection and retroperitoneal lymphadenopathy are necessary to
obtain optimal cytoreduction. Optimal cytoreduction is achieved when the largest residual tumor mass measures less than 1.5 cm. This has to be followed up with chemotherapy. Sometimes the tumour appears inoperable at first laparotomy. These patients are first given chemotherapy and when the tumour is more amenable to surgery, cytoreductive surgery should be attempted.
Germ cell tumours: Germ cell tumours include: dysgerminoma, endodermal sinus tumor, embryonal carcinoma, polyembryoma, choriocarcinoma, teratoma, mixed forms, and gonadoblastoma.
Benign germcell tumours: These are Gonadoblastoma, Mature teratoma (Dermoid), & Struma ovarii.
Malignant Germcell tumours: These include dysgerminoma, endodermal sinus tumor, embryonal carcinoma, polyembryoma, choriocarcinoma, teratoma, mixed forms, and gonadoblastoma.
Nondysgerminomatous malignancies: Unilateral tumors are the rule in nondysgerminomatous germ cell malignancies. Because of this, unilateral oophorectomy should be performed. This would preserve the contralateral ovary, as long as it appears normal, for hormone production and future childbearing potential. . Cytoreductive surgery for advanced disease should be undertaken when possible. In patients needing to preserve childbearing function, unilateral salpingo-oophorectomy should be done followed by chemotherapy. Normal menstruation is known to resume on stopping chemotherapy. There is hardly any role for second look laparotomy for follow up of germcell tumours. Measuring tumour markers may be enough for follow up.
Stage IB onwards: If the patient has completed child bearing, TAH with BSO may be done. Data are limited on treating patients with advanced or recurrent stromal tumors because of the rarity, multihistologic patterns, and indolent behavior of these tumors. Even less information is available regarding which patients should receive adjuvant therapy. However, use of chemotherapy and even radiotherapy has been described in a few studies for recurrent tumours.
Unilateral salpingo-oophorectomy may be enough for patients with with the following tumours:
- Grade I, stage 1A Invasive epithelial tumors.
- Borderline tumors.
- Germ cell tumors.
- Stromal cell tumors.
References:
- Holzer.RA,Persons.RK.,Evaluation of ovarian cysts: American family physician: Volume 84, Number 3 ◆ August 1, 2011.
- Drake J. Diagnosis and management of the adnexal mass. Am Fam Physician. 1998;57:2471-2475.
- Joshi.M,et al, Sonography of adnexal masses: Ultrasound Clin 2 (2007) 133–153.
- Beretta P; Franchi M et al. Randomized clinical trial of two laparoscopic treatments of endometriomas: cystectomy versus drainage and coagulation. Fertil Steril 1998 Dec;70(6):1176-80.
- Busacca M; Marana R Recurrence of ovarian endometrioma after laparoscopic excision. Am J Obstet Gynecol 1999 Mar;180(3 Pt 1):519-23
- Flynn MK; Niloff JM Outpatient minilaparotomy for ovarian cysts. J Reprod Med 1999 May;44(5):399-404
- Gabriel oeslner,MD et al., Long term follow up of the twisted ischaemic adnexa managed by detorsion:Fertility and Sterility Vol.60 No6 December,1993.
- Goldstein SR. Conservative management of small postmenopausal cystic masses. Clin Obstet Gynecol.1993;35:395-401.
- Guerriero S; Mallarini G. et al. Transvaginal ultrasound and computed tomography combined with clinical parameters and CA-125 determinations in the differential diagnosis of persistent ovarian cysts in premenopausal women. Ultrasound Obstet Gynecol 1997 May;9(5):339-43.
- Lee EJ; Kwon HC. Diagnosis of ovarian torsion with color Doppler sonography: depiction of twisted vascular pedicle. J Ultrasound Med 1998 Feb;17(2):83-9
- Lee EJ; Kwon HC,et al: Diagnosis of ovarian torsion with color Doppler sonography: depiction of twisted vascular pedicle.J Ultrasound Med 1998 Feb;17(2):83-9.
- Linda Van Lee,“Clinical presentation of adnexal masses” at 48th annual meeting of American College of Obstetricians and Gynecologists, San Fransisco,May 2000.
- Schutter EM, Kenemans P, Sohn C, et al. Diagnostic value of pelvic examination, ultrasound, and serum CA125 in postmenopausal women with a pelvic mass. An international multicenter study. Cancer. 1994;74:1398-1406.
- Stark JE; Siegel MJ Ovarian torsion in prepubertal and pubertal girls: sonographic findings. Am J Roentgenol 1994 Dec;163(6):1479-82.
- Troiano RN; Taylor KJ . Sonographically guided therapeutic aspiration of benign-appearing ovarian cysts and endometriomas. Am J Roentgenol 1998 Dec;171(6):1601-5.Volume 46 • Number 3 • June 1999
- Zanetta G; Lissoni A. et al., Role of puncture and aspiration in expectant management of simple ovarian cysts: a randomised study. BMJ 1996 Nov 2;313(7065):1110-3.
Stem Cells Cysts
Posted On April 26, 2018 by Dr.Shobhana Mohandas
Stem cells are primitive cells that give rise to other types of cells. Cell therapy using stem cells is a group of techniques, or technologies, that rely on replacing diseased or dysfunctional cells with healthy, functioning ones. These new techniques are being applied to a wide range of human diseases. The commonest stem cell therapy that the physician is familiar with is bone marrow transplant. Cord blood being a rich source of stem cells, there is increasing interest in the storage and use of cord blood as a source of stem cell therapy. Embryonal stem cells, derived from the human embryo is a more versatile type of stem cell, and amidst ethical problems and technical problems regarding the delay in culturing a cell line, is another source of stem cell, which is being sought for, in stem cell therapy. The use of cord blood and human embryos for this therapy brings the gynaecologists into focus as potential helpers in providing these sources of stem cells.
What are stem cells?
Stem cells are special types of cells having remarkable ability for self-renewal and they remain undifferentiated for indefinite periods of time, remaining as “reserve” cells in the body.
Types of cells in the body:
Totipotent cells are considered the “master” cells of the body because they contain all the genetic information needed to create all the cells of the body plus the placenta. Human cells have this capacity only during the first few divisions of a fertilized egg. After 3 – 4 divisions of totipotent cells, there follows a series of stages in which the cells become increasingly specialized.
Pleuri potent cells are a result of the next stage of division. These are highly versatile and can give rise to any cell type except the cells of the placenta.
Multipotent cells are at the next stage, meaning they can give rise to several other cell types, but those types are limited in number. An example of multipotent cells is hematopoietic cells—blood stem cells that can develop into several types of blood cells, but cannot develop into brain cells. At the end of the long chain of cell divisions that make up the embryo are “terminally differentiated” cells—cells that are considered to be permanently committed to a specific function.
Difference of stem cells from other cells in the body:
The other types of cells in the body are adult somatic cells, germ cells and embryonic cells. The difference between adult somatic cells and stem cells is that, adult somatic cells, once differentiated, cannot change their speciality,e.g., adult liver cell cannot perform the function of an adult pancreatic cell. Stem cells divide but do not differentiate or specialize unless directed to do so under specialized environments either “in-vivo” or “in vitro”.
Types of stem cells: Two types of stem cells have been identified.
- Adult somatic stem cells, which can be unipotent or multipotent.
Unipotent cells are those, which are capable of repairing or regenerating the tissues or organ in which they exist.
Multipotent stem cells are those that can differentiate into cells within the same family. For e.g., Haemopoetic stem cells can form all blood cells like RBC, WBC, Platelets, but not liver cell. Haemopoetic stem cells, bone marrow, mesenchymal stem cells, neural stem cells, skin stem cells, etc are examples of adult somatic stem cells.
- Embryonic stem cells, which are pleuripotent.
Uses of stem cells:
Since the 1980s, human hematopoietic stem cells have been isolated from bone marrow and used to treat patients with various hematologic malignancies. Bone marrow transplantation also has been used successfully to treat immune deficiencies, hemoglobinopathies, and metabolic diseases. Hospitals in India treating Bone Marrow Transplants are; Manipal Hospital (Bangalore), Apollo Hospitals (Chennai) and Indraprastha Apollo Hospital (New Delhi).
Myocardial infarction and other cardiac conditions:
Stem cells are delivered to the heart through an intracoronary catheter. Once the stem cells have reached areas of infarcted myocardium, they may improve contractility by differentiating into functional cardiac myocytes and improve perfusion by releasing cytokines that induce angiogenesis. The results have been positive in certain trials and without effect in others. In some patients, newly developed zones of myocardium have developed intrinsic electrical activity that spurred malignant ventricular arrhythmias, requiring placement of an implantable cardioverter defibrillator.
In India work in this area was pioneered at All India Institute of Medical sciences, Delhi. Many patients with this conditions are being given stem cell therapy in Asian Heart Institute & Research Centre, NiCRM, Nizam’s Institute of Medical Sciences (NIMS) , Frontier Lifeline Hospital, Chennai, Tirupati-based C Venkateswarlu Institute for SCT, & Manipal Education and Medical Group’s (MEMG). Phase I multi-centric clinical trial using bone marrow mononuclear cells on acute myocardial infarction are going on at five hospitals in the country, that is, CMC; Sanjay Gandhi Post Graduate Institute for Medical Sciences (SGPGIMS), Lucknow; Post Graduate Institute of Medical Education & Research (PGIMER), Chandigarh; Research & Referral Hospital, New Delhi; Air Force Medical College (AFMC), Pune and All India Institute of Medical Sciences (AIIMS), New Delhi.
Alzheimer’s disease, Parkinson’s disease, Multiple sclerosis, Spinal injuries:
Animal studies have found stem cells useful in neurological diseases. Adult stem cells from bone marrow or adult tissues, without viral contamination could be used for this. If embryonal tissues are used, it should be less than 14 days old prior to formation of neural tissue. Stem cell therapy for paraplegics following spinal injury is being done at Global hospital, hyderabad as an ICMR project. . The pilot study on acute ischemic stroke has also been initiated at AIIMS. Reliance Life Sciences, Mumbai has characterised 10 stem cell lines, including two neuronal cell lines, dopamine producing neurons and neurons for patients of stroke.
Disorders of the eye: In one of the programmes at L V Prasad Eye Institute (LVPEI), Hyderabad, limbal stem cells are being used to repair the cornea surface.
Paediatric conditions: Fanconi’s anaemia and some metabolic disorders have successfully been treated using cord blood stem cells. Cord blood is more readily accepted for paediatric cases as compared to adult patients. This is because, children have a smaller physical size and the stem cell dose will be smaller and easily available from the cord units even if the number of stem cells present in them are limited.
Others: stem cell therapy holds promise for many other conditions like type-1 diabetes, burns,and research is being done on stemcells to produce sperms, obviating the need for sperm banks.
Sources of stem cells:
Adult stem cells (AS): Hematopoietic stem cells are present in the bone marrow and circulating blood. These cells are readily accessible. Other rare, hard to identify AS cells are scattered throughout the body. Stem cells from bone marrow take 3 weeks to culture.
Cord blood stem cells: Normally, cord blood is collected before the placenta is delivered. A baby’s umbilical cord blood, which is otherwise discarded, is a rich source of stem cells endowed with the ability to regenerate and replace a variety of tissues. In recent years, the concept of cord banking is catching on in India. Interestingly, banking cord blood in a cord blood bank is considered a “biological insurance” since the child from whose umbilical cord the blood is collected can ostensibly stand to benefit from it at any stage of his life. We however do not have enough cord blood banks that have stored blood for more than 20 years or so and so it remains to be seen if such blood can be used life-long. We have to see whether cell lines can be maintained so long keeping their inherent capacity to function as stem cells intact.
There are blood banks which offer to store baby’s cord blood in liquid nitrogen for a period 21 years for a fee of around Rs.60, 000. The Chennai-based Cryocell has set up facilities to preserve cord blood. Similarly, Life cell, yet another private stem cell bank in Chennai says that about 1,000 expectant parents have enrolled to bank the cord blood stem cells. The recently-set up Bangalore-based Cryostem Karnataka Pvt Ltd is a cord blood stem cell bank as well as research centre. The other cord blood banks in India are Reliance life sciences, Mumbai,and Asia life cell Pvt Ltd, Chennai,.
The pure stem cells are then separated from the rest of the cord blood with a patented technology, and are cryogenically frozen in vials, under strict laboratory conditions. These Cord Blood Stem Cells are pure, with no red or white cells. This negates the need for blood typing or HLA matching, safe, with no graft versus host or rejection issues (as is the potential from whole cord blood). Pluripotent, CBSC have been proven to regenerate every single cell in the human body. (C. Verfaillie, Univ. of Minnisotta July 2002).
In most cases, Cord Blood Stem Cells Therapy involves one simple IV (intravenous) injection. Once in the body, the cells migrate to the site of disease and begin replacing damaged or missing cells. This process of noticeable reconstitution usually peaks between 3 and 6 months following treatment. Often significant results are noted at the one-month mark. Cord blood is a reasonable graft source for adults who cannot find an HLA match in a bone-marrow registry or who need transplantation sooner than the 3–4 months needed to obtain unrelated adult-donor bone marrow.
Embryonal stem cells (ESC): Embryonal stem cells are pleuripotent.
Embryonal cells can be taken from the inner cell mass(ICM) of the blastocyst around days 5–6 after fertilization in mouse and days 8–9 in humans, isolated and put in culture. The trophectoderm is removed and the inner cell mass (ICM) is plated on to a feeder layer of mouse or human embryonic fibroblasts, which is essential for the survival of the ICM. The ICM then flattens into a compact colony of ESCs, which is than mechanically dissociated and re-plated several times to give rise to stable cell line. When cultured in the laboratory, human ESCs grow as compact colonies and usually require the presence of feeder cells for their survival. When undifferentiated human ESC colonies are detached from the feeder layer and transferred into serum containing medium, they form multi-cellular aggregates called embryoid bodies (EB) which can contain cell types representing all three germ layers of the body: endoderm, mesoderm, and ectoderm.
Somatic cell nuclear transfer: Human ova are denuded of their neucleus and the neucleus from a patient’s cell is transferred in to the ovum. It develops into an embryo and the inner cell mass is taken from its blastocyst and stem cells cultured from it. This method has the advantage of using the patient’s own cells with no potential of immune rejection and the stem cell being genetically identical to cell source. People who believe that life starts before conception are against the idea of growing human embryos and destroying them, because human embryos according to them could be potential human beings.
Disadvantage: Culturing human embryonal stem cells can take up to 6 months and it may be too long a period for critically ill persons who are looking up to stem cell therapy as a last resort therapy.
Stem cell therapy and the gynaecologist
The gynaecologist, especially in charge of IVF centres could be approached for embryos or ova, which could be cloned to form embryos, which are a source of pleuripotent stem cells. Obstetricians could be approached by cord blood banks to make people more aware of the advantages of storing their baby’s cord blood, which could be used any time in the next 20 or so years, should the baby face the contingency of suffering from any haematologic/metabolic condition requiring stem cell therapy during that time. Women with history of relatives suffering from such conditions could approach the obstetrician with a request to store the cord blood of her baby.
Stem cell nuclear transplant or cloning of ova is still controversial as many people find it repulsive to manipulate potential human beings for research even if they are in the embryonic form. Culturing embryonal cells take a long time and till this period is shortened, using embryonal cells to form useful stem cells for therapy should be considered a research project as far as humans are concerned. Animal studies have been encouraging.
Conclusion : the media being very active about propagating information about the uses of cord blood, every obstetrician should know the centres with cord blood banks and the method of collecting, storing and dispatching cord blood to such centres.
